Objective: Complete urinalysis (CUA) is one of the indispensable screening tests of clinical laboratories. The compatibility of this test with urine culture is of indispensable importance in the diagnosis and treatment of urinary tract infections. We aimed to evaluate the suitability of the leukocyte parameter measured in the microscopic units of the fully automated urine analyzers which replace traditional methods, by grouping them according to the results of chemical analysis.
Materials and Methods: Leukocyte counts in the reported CUA results of 4685 outpatients and the results of 113 urine cultures studied on the same day were analyzed. Noncentrifugated urine samples were included in the analysis. Cells were digitally imaged by flow microscopy. Chemical analyzes were performed using dual wavelength reflectance method. Urine samples were evaluated after 24 hours of incubation.
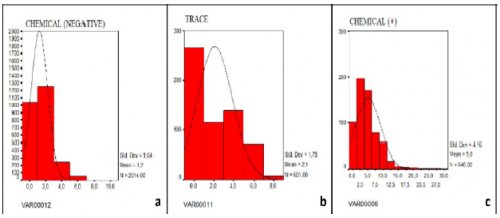
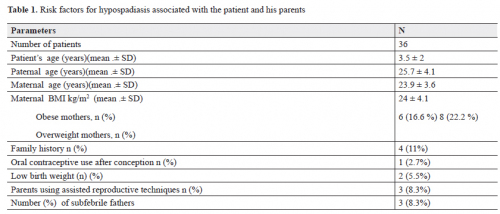
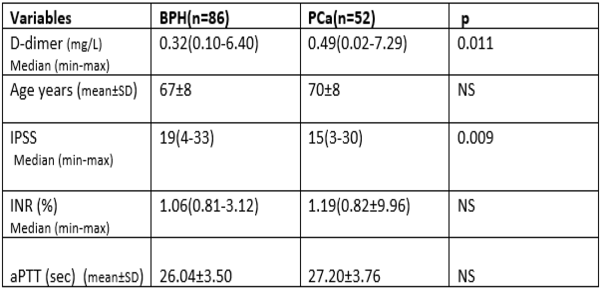
Results: High power field (HPF) values were recorded by grouping the leukocyte counts as negative, trace, 1+, 2+ and 3+. The arithmetic means of HPF values of the groups were calculated as 1.2, 2.1, 5.0, 11 and 208 white blood cell (WBCs/HPF). Bacterial growth was detected in 19 of 113 patients and no reproduction was observed in the remaining 94 cases. When results of microscopic examinations and chemical analysis were compared with the culture results, the analytical sensitivity, specificity, positive, and negative predictive values for microscopic urinalysis were 25%, 86%, 61.3%, and 58.3%, respectively. While, the analytical sensitivity, specificity, positive, and negative predictive values for chemical analysis of urine were 25.8%, 87.7%, 69.7%, and 51.4%, respectively.
Conclusion: The workload of medical laboratories is increasing, and the use of urine autoanalyzers may be preferred for busy laboratories. In the diagnosis and follow-up of urinary tract infections, complete urinalysis by autoanalysers in which the harmony of their microscopy and chemical units are closely monitored, may reduce the need for unnecessary requests for urine culture, but it cannot replace urine culture.